By Sarah Edmonds and Heather F. McClintock
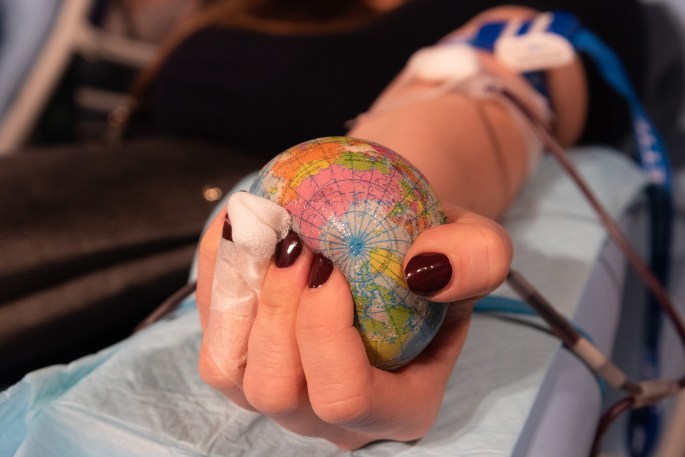
As we look back on the month of June, which has played host to World Blood Donor Day, Pride Month in the USA, and an unrelenting continuation of COVID-19 and its variants, the time has never been better to discuss the need for and barriers to high rates of blood donation worldwide.
In order to maintain safety procedures during this pandemic, blood drives and many blood donation services were cancelled; this, paired with increased hospitalization rates and the investigation of plasma treatments for COVID-19 led to one of the worst global blood shortages in recent history. In some countries, blood donation rates dropped by a massive 40%. Based on the US Food and Drug Administration (FDA) recommendations, men who had sex with other men (MSM) within the past year were ineligible to donate and were required to stay celibate for at least a year to regain eligibility. However, on April 3, 2020 due to the deteriorating blood supply, as well as pressure from the media and various advocacy organizations, the FDA shortened the blood donation deferral period for MSM from 1 year to 3 months. With the new 3 month deferral period many MSM sought to donate blood in the United States. However, despite the changed FDA recommendations, many MSM were turned away from donating blood based on their sexual practices even though they were legally within their bounds to do so in the United States.
Other nations, such as Italy and Spain, determine risk and deferments based on self-reported questionnaires which, depending on results, may completely ban individuals from ever donating blood at all. In contrast, Argentina implemented in 2015 a “gender neutral” risk-based approach that did not enforce policies based on sexual orientation or gender identity. This policy demonstrated no significant difference in the prevalence of HIV in spite of a substantial increase in the number of donors. This finding provides substantive evidence that an inclusive blood donor policy does not result in an increased risk of HIV in the blood supply.
Reevaluating the processes and biases in the process of screening blood donors in the United States would potentially allow for countless willing and healthy donors—who would under current policies be turned away—to help fight the ongoing blood shortage. Many organizations such as the National Alliance of State and Territorial AIDS Directors and the HIV Medicine Association have called for a complete rescission of the deferral period. Park et al. proposed an eligibility screening format that involves an individual risk-based screening protocol. This approach would not exclude donors based on gender identity or sexual orientation. This approach supports the equitable treatment of marginalized community members as blood donors while maintaining health and safety outcomes.
As was the theme with the June 14th World Blood Donor Day, giving blood keeps the world beating. By making blood donation sites more abundant, more accessible, and more mobile we can be sure to see a marked increase in willing donors. Above all, we can and must make blood donation accessible and viable (with equitable access regardless of sexual orientation) for as many willing unpaid donors as possible in order to fight this blood shortage and to continue saving lives in the future.