Politics & Policies
A new study that examines some major health care proposals from presidential candidates finds that Donald Trump would cause about 20 million to lose coverage while Hillary Clinton would provide coverage for an additional 9 million people.
The government isn’t regulating how highly dangerous viruses and bacteria are rendered safe for shipment, posing risks to the public, auditors say.
At this year’s United Nations General Assembly, policymakers and elected officials should increase their political commitment for breast- feeding as they work to tackle issues of critical importance related to the health, wellbeing and economic success of their 193 states. It’s directly related to our collective goals.
The United States unveiled plans on Thursday to ramp up efforts to end female genital mutilation (FGM) after figures showed more than half of million women and girls were living at risk.
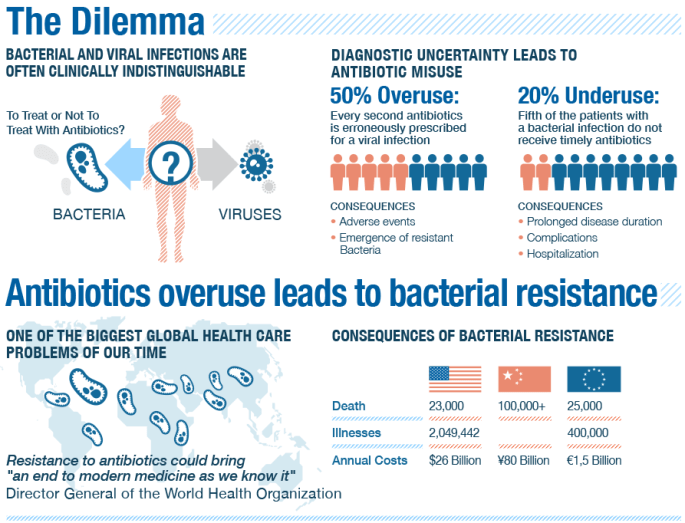
On September 21st in New York all 193 UN member states agreed to tackle the growing resistance of microbes to antibiotics. Drug-resistant infections now kill more than 700,000 people a year. On current trends, that number may reach 10 million by 2050.
Senate Republicans on Thursday released the latest draft of a $1.1 billion funding package to fight the Zika virus, and it contains some of the controversial funding offsets that Democrats have long opposed.
The World Health Organization (WHO) is preparing to select a new director general. It needs someone dynamic and politically astute to drive strategic reforms, say global health experts.
A study funded by the Bill and Melinda Gates Foundation, measured how countries, including Australia, China, India, the US and UK, performed over the last 15 years with Iceland taking the top spot for its health related Sustainable Development Goal (SDG) performance.
New Zealand falls way behind our neighbours across the Tasman as a healthy country to live in, a major global study has found.
Programs, Grants & Awards
The Center for Global Health in the Perelman School of Medicine at the University of Pennsylvania is pleased to honor Ernest Madu, MD, chairman and CEO of the Heart Institute of the Caribbean with its first annual Global Health Champion Award. Madu was presented with the award on Thursday, Sept. 15 as part of a celebration for Penn’s newly launched Center for Global Health.
Bill Gates, Bono among big names at Montreal conference to replenish fund to fight HIV/AIDS, TB and malaria.
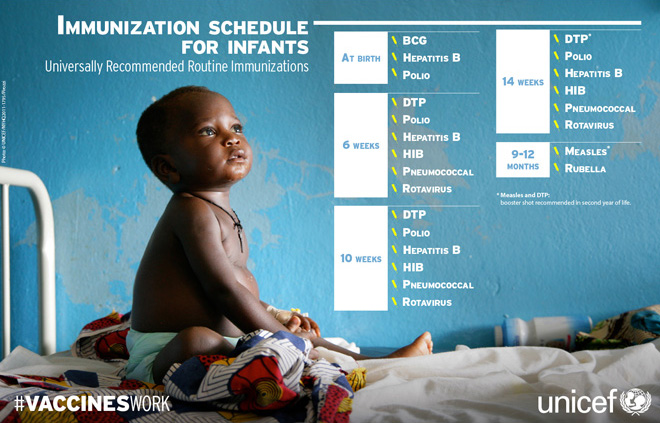
Glaxo-Smith Kline (GSK) has plans to address emerging global health issues, the company said in a Sept. 19, 2016 press release. The company put forth a series of steps it will take in order to combat several global health challenges, including access to vaccines, antimicrobial resistance, and preparation for future pandemics.
University of Iowa students now will be able to expand their knowledge of health around the world, thanks to a new major in Global Health Studies.
Research
Since December 2013, an armed conflict in South Sudan has resulted in the displacement of over 2.2 million people, more than 270,000 of whom are presently in refugee settlements located throughout Uganda. Existing literature suggests that refugees are at increased risk for a range of mental health and psychosocial problems.
Molecular surveillance identifies multiple transmissions of typhoid in West Africa.
Experimental treatment of Ebola virus disease with brincidofovir.
During 2004–2013 in Mozambique, 455,600 HIV-positive adults (≥15 years old) initiated antiretroviral therapy (ART). We evaluated trends in patient characteristics and outcomes during 2004–2013, outcomes of universal treatment for pregnant women (Option B+) implemented since 2013, and effect on outcomes of distributing ART to stable patients through Community ART Support Groups (CASG) since 2010.
Informed risk assessment and decision making for an emerging infectious disease in the Asia-Pacific Region.
For the first time, abnormal brain development following a Zika infection during pregnancy has been documented experimentally in the offspring of a non-human primate.
By 2050, 75% of the world’s population is expected to live in cities, making city planning key for addressing disease prevention and global health challenges, according to a series published in The Lancet.
Diseases & Disasters
Hookworm is a parasite that is behind millions of infections worldwide. This intestinal parasite can cause a host of complications in people of all ages.
More than a third of the burden of disease experienced by Indigenous Australians could be prevented, with tobacco and alcohol use, high body mass, physical inactivity, high blood pressure and diet contributing to their illnesses, data released by the Australian Institute and Health and Welfare shows.
Miami district which saw the first locally transmitted Zika cases in the US has been declared free of the virus.
Health organizations have all the right weapons to eradicate polio, but can’t deploy them because of wartime conflict in Nigeria, Pakistan and Afghanistan – the last three countries affected by the disease.
The World Health Organization (WHO) has recently initiated a global health strategy, which will run between 2016 and 2021, to eliminate hepatitis C as a global health threat by 2030.
With all four strains of the dengue virus now circulating in Pakistan and outbreaks of the viral disease being reported in new areas, this South Asian country now faces a serious health problem from the mosquito-borne pestilence, researchers say.
In the five years since the civil war between President Bashar Assad’s government and rebel groups began, more than 250,000 Syrians have died in the conflict. But thanks to the White Helmets, over 60,000 lives have been saved.
Traditional strategies for delivering health services to refugees and migrants will not meet the needs of today’s 65 million displaced people, according to refugee, development and global health experts who met Thursday at a UN General Assembly side event.
Technology
A new technique may democratise vaccine production. James Collins of the Massachusetts Institute of Technology (MIT) thinks that he may have developed one.
Healthcare, the USD 18-billion healthcare technology unit of GE, has announced USD 59-million funding aimed at improving services of healthcare startups in developing countries.
Facebook founder Mark Zuckerberg and his wife Priscilla Chan have pledged $3 billion (£2.3bn) to fund medical research over the next decade. At a press conference in San Francisco, they said their ultimate goal was to “cure, prevent or manage all diseases by the end of the century.”
Environmental Health
Volkswagen (VW) emissions cheat may lead to 50 premature deaths, $423 million in economic costs, study shows.
Australia’s offshore petroleum industry regulator is set to rule next week whether to grant oil giant BP’s application to drill in the Great Australian Bight.
While July was busy becoming the hottest month in 136 years of record-keeping, Donald Trump made no reference at all to climate change in his nomination-acceptance speech, and Hillary Clinton made only two passing references in hers.
A week before Russia’s Daldykan river was turned red by a leak from a metals plant, the UN issued a warning as chilling as it was overlooked: 323 million people are at risk from life-threatening diseases caused by the pollution of rivers and lakes.
Equity & Disparities
Gender equality remains the greatest human rights challenge of our time, and one way to achieve the goal is by empowering women to have greater choices economically and control over their lives, United Nations Secretary-General Ban Ki-moon declared today, urging the international community to spearhead efforts that provide opportunities for women and girls.
A new analysis shows that the life expectancy of people living with HIV is very different between Europe, North America and African countries. The analysis pools the results of eight previously published studies on life expectancy, with over 150,000 people included.
Increasing evidence from scientists the world over indicates that many health outcomes — everything from life expectancy to infant mortality and obesity — can be linked to the level of economic inequality within a given population. Greater economic inequality appears to lead to worse health outcomes.
The global news round up was prepared by the communications team.